Understanding the Dignity Gap: How Family Caregivers Navigate the Transition to Personal Care
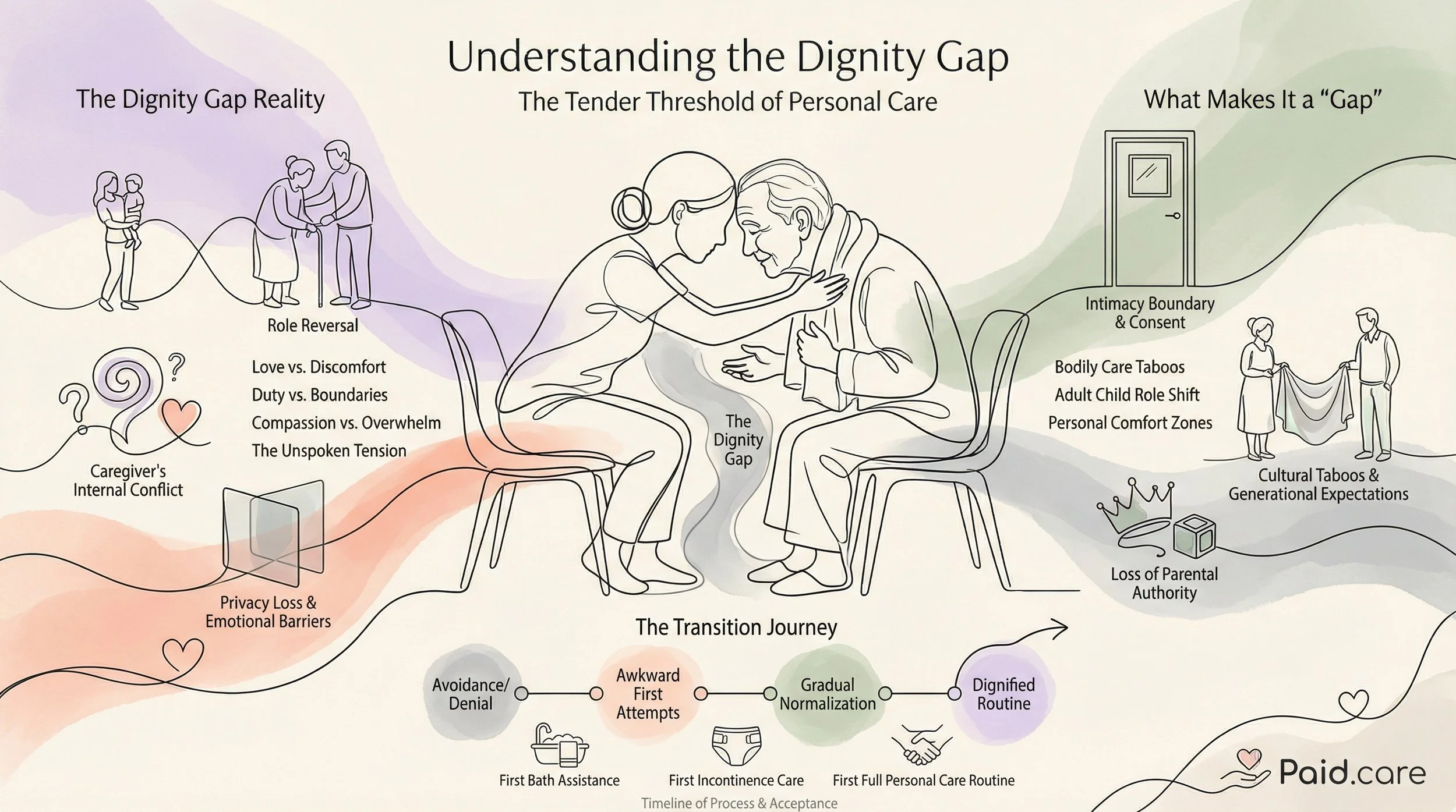
The transition to personal care for elderly loved ones often reveals a significant challenge known as the "Dignity Gap." This term encapsulates the emotional and practical struggles faced by family caregivers as they navigate the complexities of providing care while maintaining the dignity of their loved ones. In this article, we will explore the implications of the Dignity Gap, the emotional challenges that arise during personal care transitions, and the support systems available to assist caregivers. We will also discuss how Medicaid and Medicaid waivers can provide essential assistance in this journey, along with practical steps families can take to manage these transitions effectively.
What Is the Dignity Gap in Elderly Care Transitions?
The Dignity Gap refers to the disparity between the care that elderly individuals require and the care that family members are able to provide. This gap often leads to feelings of inadequacy among caregivers, who may struggle to meet the emotional and physical needs of their loved ones. Addressing this gap is crucial, as it not only affects the quality of care but also the emotional well-being of both caregivers and care recipients. Understanding the Dignity Gap helps families recognize the importance of support systems and resources available to them.
How Does the Dignity Gap Affect Family Caregivers and Loved Ones?
Family caregivers often experience significant emotional tolls due to the Dignity Gap. The pressure to provide adequate care can lead to feelings of guilt, anxiety, and frustration. These emotions can strain family dynamics, as caregivers may feel isolated in their struggles. It is essential for caregivers to seek support from community resources, support groups, and mental health services to mitigate these challenges. By addressing their emotional needs, caregivers can better support their loved ones and maintain healthier family relationships.
What Emotional Challenges Arise During Personal Care Transitions?
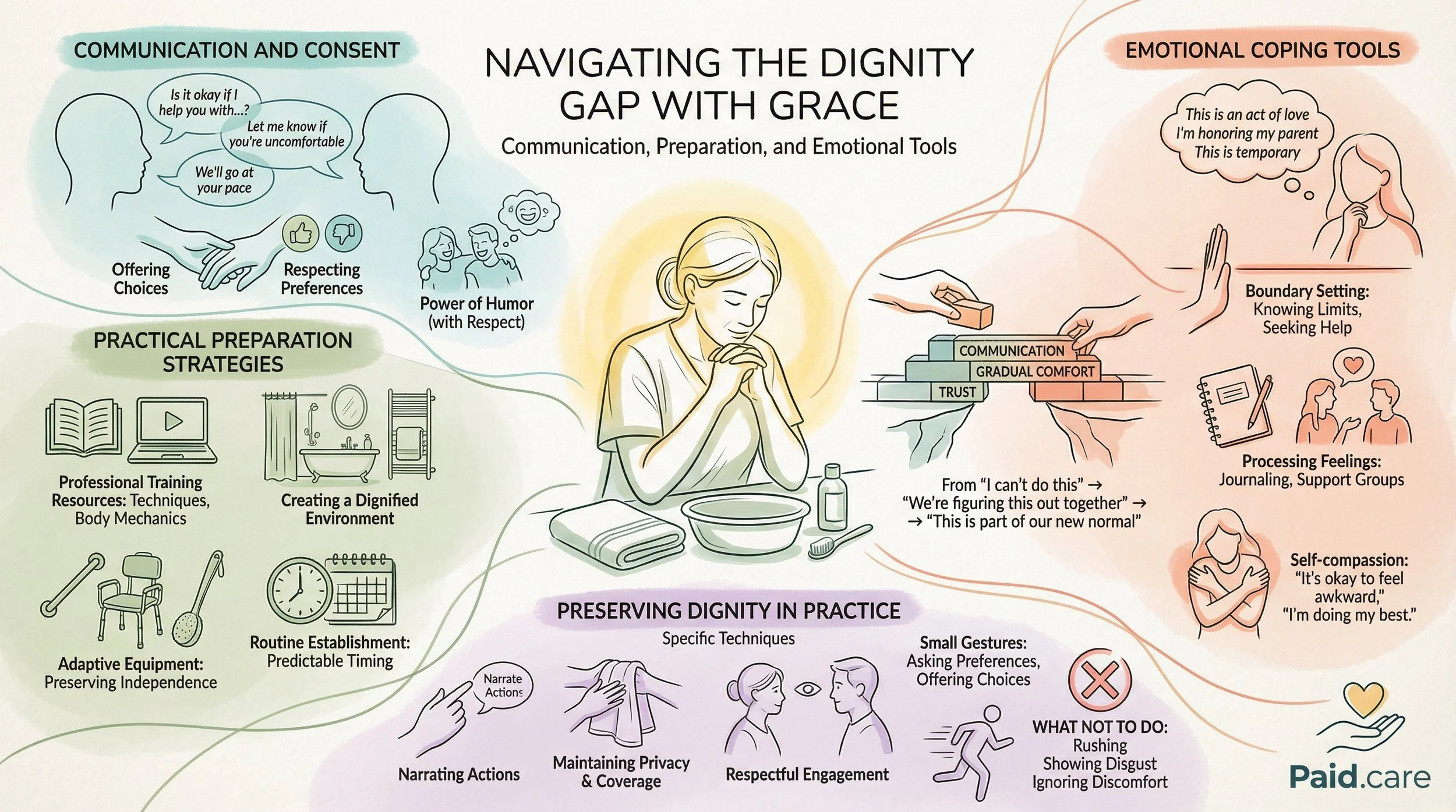
During personal care transitions, caregivers frequently encounter emotional challenges such as guilt and anxiety. Guilt may stem from the feeling that they are not doing enough for their loved ones, while anxiety can arise from the uncertainty of navigating new caregiving responsibilities. Coping mechanisms, such as mindfulness practices and seeking professional support, can be beneficial in managing these feelings. Recognizing the importance of mental health support is vital for caregivers to sustain their well-being and effectiveness in their roles.
How Do Medicaid and Medicaid Waivers Support Personal Care Assistance?
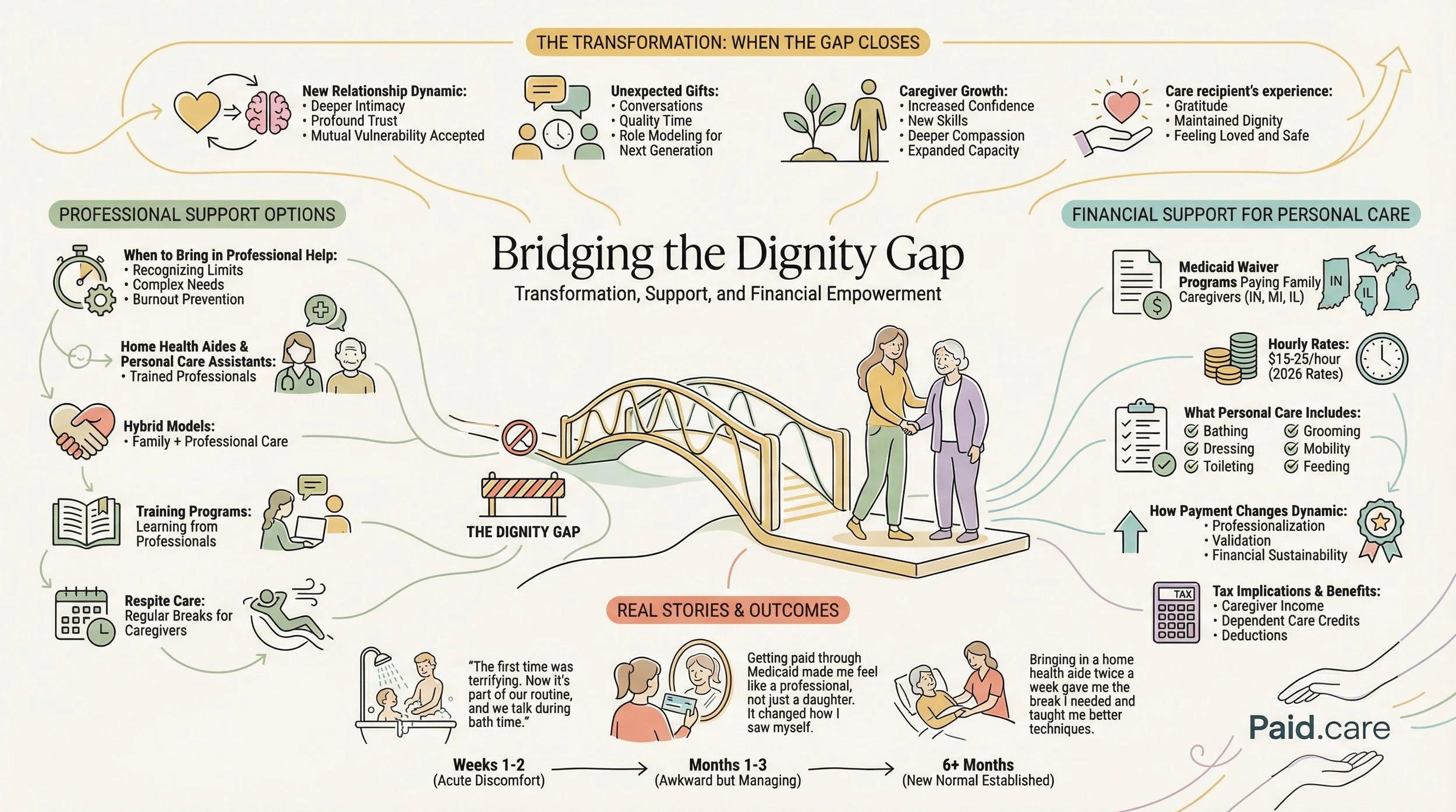
Medicaid and Medicaid waivers play a crucial role in supporting personal care assistance for families navigating the Dignity Gap. These programs provide financial assistance for home care services, allowing families to access the necessary support without incurring overwhelming costs. Understanding how these programs work can empower caregivers to make informed decisions about their loved ones' care.
What Are the Eligibility Criteria for Medicaid Home Care in Indiana, Michigan, and Illinois?
Eligibility criteria for Medicaid home care vary by state, but generally include factors such as income, asset limits, and medical necessity. In Indiana, for example, applicants must meet specific income thresholds and demonstrate a need for assistance with daily living activities. Michigan and Illinois have similar requirements, but the details can differ significantly. Families should consult local Medicaid offices or resources to understand the specific criteria applicable in their state.
How Can Family Caregivers Apply for Medicaid Waivers in These States?
Applying for Medicaid waivers can be a complex process, but understanding the steps involved can simplify it for family caregivers. Typically, the application process includes gathering necessary documentation, such as proof of income and medical assessments. Caregivers should also be prepared to navigate potential waiting lists for services. Seeking assistance from local advocacy groups or social workers can provide valuable guidance throughout the application process.
What Practical Steps Help Families Plan and Manage the Transition to Personal Care?
Effective planning is essential for families managing the transition to personal care. By taking proactive steps, families can ensure a smoother transition and better outcomes for their loved ones. This includes creating comprehensive care plans, identifying available resources, and establishing open communication among family members.
Which Checklists and Resources Guide Long Term Care Planning?
Families can benefit from various checklists and resources designed to guide long-term care planning. These resources often include lists of questions to consider when evaluating care options, as well as information on local services and support networks. Utilizing these tools can help families make informed decisions and feel more confident in their caregiving roles.
How Can Caregivers Access Emotional and Financial Support Services?
Accessing emotional and financial support services is crucial for caregivers facing the challenges of the Dignity Gap. Many organizations offer resources such as counseling, support groups, and financial assistance programs. Caregivers should actively seek out these services to alleviate stress and enhance their ability to provide care. By leveraging available support, caregivers can improve their own well-being and the quality of care they provide to their loved ones.
FAQs
-
The Dignity Gap is the psychological and emotional tension that occurs when a senior transitions from independence to needing help with intimate "Activities of Daily Living" (ADLs), such as bathing, dressing, and toileting. For a family caregiver, this gap is the space between the physical necessity of the task and the recipient’s need to feel like an autonomous adult. Navigating this requires shifting your mindset from "performing a task" to "preserving personhood," ensuring that the care doesn't make the loved one feel like a "patient" in their own home.
-
The most effective strategy is "Consent-Based Care" combined with the "Choice Architecture" model. Instead of dictating a schedule, offer micro-choices that empower the senior, such as asking, "Would you like to get dressed before or after breakfast?" or "Would you prefer the blue or grey outfit today?" In 2026, caregivers are also bridging the gap with "Least Restrictive Supports"—using tools like high-end bidet attachments or specialized grooming aids—which allow the senior to maintain privacy for the most sensitive parts of their routine for as long as possible.
-
Yes. Under 2026 Medicaid "Self-Directed" or "Participant-Directed" waivers, a senior can often choose to have a family member or friend paid to provide personal care. This is a major win for dignity, as it allows the senior to receive help from a trusted person rather than a stranger. However, under the 2026 federal H.R. 1 guidelines, you must maintain a "Caregiver Evidence Log" that specifically documents which ADLs were performed and when. This documentation is required both for your payment and to ensure the caregiver is exempt from state-level "Community Engagement" work requirements.
-
The rise of "Passive Monitoring" in 2026 has revolutionized personal care. Rather than a caregiver needing to check in physically every hour—which can feel intrusive—AI-driven smart home sensors and wearables can now detect if a senior is struggling in the bathroom or has missed a medication. This allows the caregiver to remain in a "support" role, only stepping in when the AI identifies a specific need. This technology acts as a digital buffer, giving the senior more "unsupervised" time and significantly reducing the "transactional" feel of the caregiving relationship.