The Solo Ager Strategy: Can Friends Get Paid as Caregivers under Medicaid?
The concept of "Solo Agers" refers to individuals who age without a partner or children to provide support. As this demographic grows, the need for caregiving solutions becomes increasingly important. This article explores whether friends can be compensated as caregivers under Medicaid, a crucial consideration for Solo Agers seeking assistance. Understanding the intricacies of Medicaid Waiver programs can empower Solo Agers to secure the help they need while navigating the complexities of caregiver compensation. We will delve into the mechanisms of Medicaid Waivers, state-specific rules in Indiana, Michigan, and Illinois, the application process for caregiver payment, and the legal and financial considerations involved.
What Are Medicaid Waiver Programs and How Do They Support Solo Agers?
Medicaid Waiver programs are state-specific initiatives that allow for flexibility in how Medicaid funds are used to support individuals needing long-term care. These programs are designed to provide services that help individuals remain in their homes rather than being placed in institutional settings. For Solo Agers, these waivers can be a lifeline, offering access to essential caregiving services that enhance their quality of life.
How Do Medicaid Waivers Enable Caregiver Payment?
Medicaid Waivers enable caregiver payment by allowing states to reimburse family members or friends who provide care. This payment structure is crucial for Solo Agers who may prefer receiving care from someone they trust rather than a professional caregiver. The reimbursement can cover various services, including personal care, companionship, and assistance with daily activities, making it a viable option for many.
What Are the Eligibility Criteria for Medicaid Waivers?
Eligibility for Medicaid Waivers typically includes several criteria, such as income limits, asset tests, and the need for assistance with daily living activities. Applicants must demonstrate that they require help to perform essential tasks, which can include bathing, dressing, and meal preparation. Additionally, documentation proving the need for care and the caregiver's qualifications may be required, ensuring that the program serves those who genuinely need it.
Can Friends Be Paid as Caregivers in Indiana, Michigan, and Illinois?
The ability for friends to be paid as caregivers varies by state, with specific rules and regulations governing the process. Understanding these state-specific guidelines is essential for Solo Agers considering this option.
What Are Indiana’s Medicaid Caregiver Reimbursement Rules?
In Indiana, Medicaid allows for reimbursement of caregivers, including friends, under certain conditions. The state has established guidelines that outline the reimbursement process, which includes submitting documentation of the care provided and meeting specific eligibility criteria. Caregivers must also undergo a background check to ensure the safety and well-being of the individual receiving care.
How Does Michigan Handle Medicaid Caregiver Payments?
Michigan has a similar approach to caregiver payments, allowing friends to be compensated for their caregiving services. The state’s Medicaid program outlines specific eligibility requirements and payment structures, ensuring that caregivers are adequately reimbursed for their time and effort. This flexibility is particularly beneficial for Solo Agers who may prefer familiar faces providing their care.
What Are Illinois Caregiver Payment Programs and Eligibility?
Illinois offers various caregiver payment programs that include provisions for friends to be compensated. The eligibility criteria often mirror those of other states, requiring documentation of care needs and the caregiver's qualifications. Understanding these programs can help Solo Agers in Illinois secure the necessary support while maintaining their independence.
How Can Friends Apply for Medicaid Waiver Caregiver Payment?
Applying for Medicaid Waiver caregiver payment involves several steps, including gathering necessary documentation and understanding the application process. This section provides guidance on how friends can navigate this system effectively.
What Documentation Is Required for Friend Caregiver Compensation?
To apply for caregiver compensation, specific documentation is required. This may include proof of the Solo Ager's need for care, the caregiver's qualifications, and any relevant medical records. Ensuring that all necessary documents are in order can streamline the application process and increase the likelihood of approval.
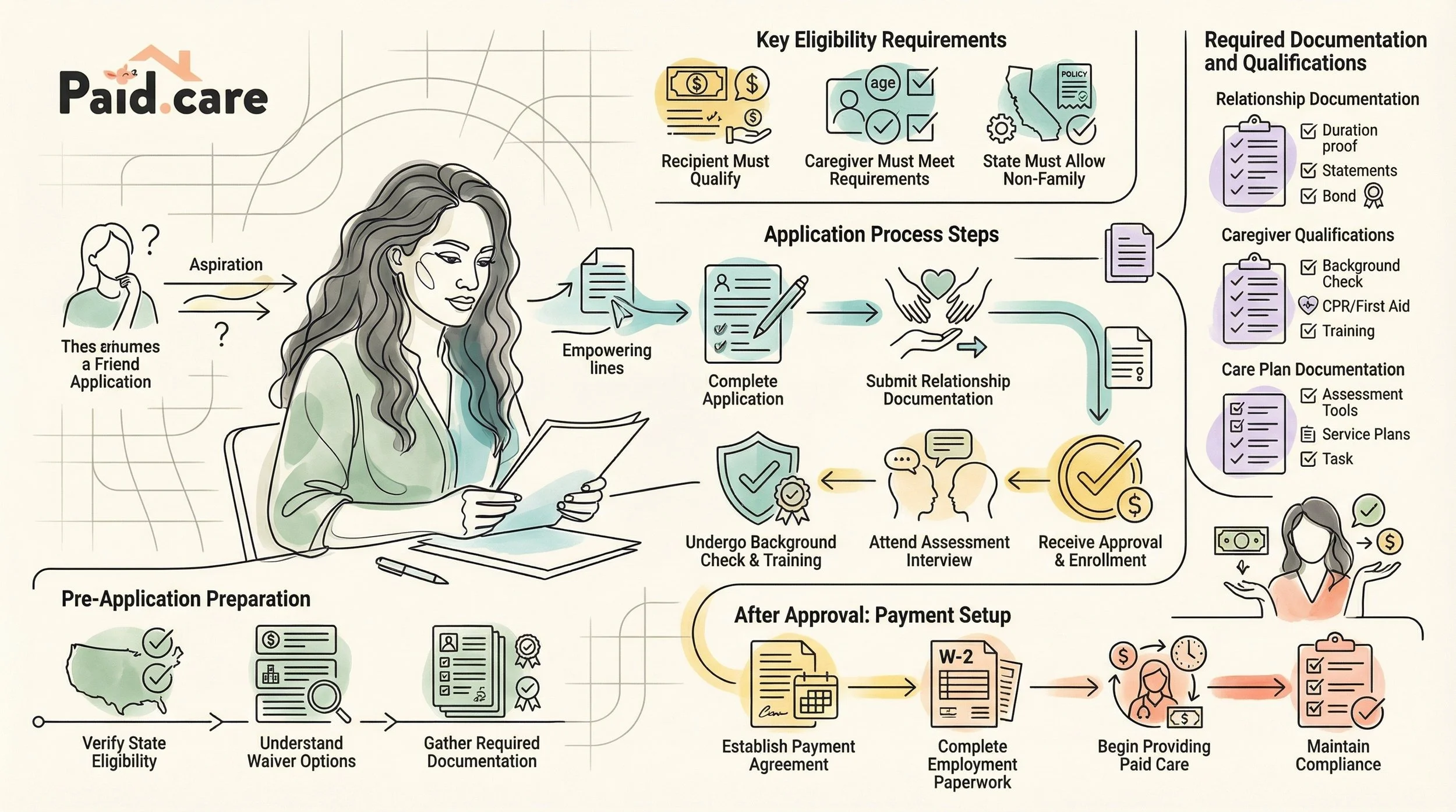
What Are the Steps to Apply for Medicaid Waiver Caregiver Payment?
The application process for Medicaid Waiver caregiver payment typically involves several key steps:
Gather Documentation: Collect all necessary paperwork, including medical records and proof of care needs.
Complete the Application: Fill out the Medicaid Waiver application form accurately, ensuring all information is correct.
Submit the Application: Send the completed application and supporting documents to the appropriate state agency.
Follow Up: Check the status of the application regularly and respond promptly to any requests for additional information.
By following these steps, friends can effectively apply for caregiver compensation under Medicaid Waiver programs.
What Legal and Financial Considerations Should Solo Agers and Friend Caregivers Know?
Navigating the legal and financial aspects of caregiver compensation is crucial for both Solo Agers and their friends providing care. Understanding these considerations can help avoid potential pitfalls.
How Do Medicaid Rules Affect Friend Caregiver Compensation Legally?
Medicaid rules play a significant role in determining the legality of friend caregiver compensation. It is essential for both the Solo Ager and the caregiver to understand the regulations governing payment to avoid any legal issues. This includes being aware of the requirements for documentation and the potential implications of non-compliance.
What Financial Planning Should Solo Agers Consider for Paid Caregiving?
Financial planning is a critical aspect of securing caregiver compensation. Solo Agers should consider their overall budget, including how much they can afford to pay for caregiving services and the potential impact on their long-term financial health. Additionally, exploring options for financial assistance through Medicaid Waivers can provide valuable support in managing caregiving costs.
FAQs
-
Yes. In 2026, nearly all states allow "Self-Directed" or "Participant-Directed" care through Home and Community-Based Services (HCBS) waivers. For a solo ager—someone without a spouse or children—this is a vital strategy. You have the right to hire a friend or neighbor to provide your care. They must typically pass a background check and may need to complete basic state-authorized training, but they do not need to be a medical professional or a relative to receive a Medicaid-funded wage.
-
Because you may not have "next of kin" to step in automatically, you must proactively name your friend as your Health Care Proxy and provide them with a Durable Power of Attorney (POA) that includes a "caregiver compensation" clause. This ensures that if you become incapacitated, your friend has the legal authority to sign their own timesheets and manage your Medicaid budget on your behalf. Without these documents, the state may appoint a professional guardian instead of your chosen friend.
-
Wages for self-directed caregivers have seen significant increases. As of 2026, many states have moved toward a $20-per-hour floor for In-Home Supportive Services (IHSS) and similar programs to combat the caregiver shortage. The exact rate is determined by your state and the "Level of Care" assessment you receive. For a solo ager, these funds allow a friend to reduce their own working hours elsewhere to focus on your care, making the arrangement sustainable rather than just a favor.
-
New federal rules implemented in 2026 (often cited under the H.R. 1 policy umbrella) have introduced stricter "Community Engagement" or work requirements for Medicaid beneficiaries. However, there is a specific exemption for caregivers. If your friend is your primary caregiver, they are exempt from these work requirements, but you must maintain meticulous documentation. This includes keeping a daily log of care tasks and ensuring your friend is officially registered with your state’s Financial Management Services (FMS) provider to avoid any eligibility red flags.